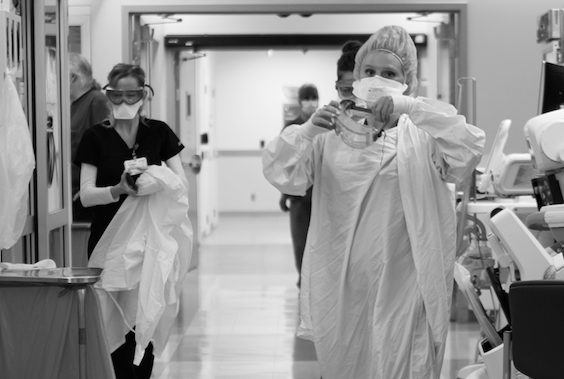
Pushed beyond their limits by increasing demands for services and a nationwide shortage of nurses, hospitals across the state are struggling more than at any other point in the pandemic to meet their communities’ need for health care.
According to Oregon Health Authority epidemiologist Dr. Dean Sidelinger, St. Charles Health System has been especially hard-hit, KTVZ reported last week.
But, “this is not a St. Charles problem. This is an Oregon problem,” said Dr. Doug Merrill, St. Charles’ chief medical officer. “One hundred percent of the hospitals in Oregon are in the same situation we are, and it’s worse than it was during some of our better-known surges over the past two years.”
The problem is two-fold: Hospitals have “shrunk,” Merrill said, because lack of staff is forcing them to close beds. The labor crisis is the result of many factors, including health care workers fleeing the industry, staff who are temporarily out because of COVID-19 illness or vacation, and a nationwide shortage of nurses that has been brewing for years due to an aging workforce, the impact of the aging Baby Boomer population’s increasing need for health care services and a nursing education system that has not grown fast enough to meet demand.
“The industry has seen this coming, and now it’s here,” said Joan Ching, chief nursing executive for St. Charles. “Retirement is a factor. Pandemic stress and burnout is a factor. But beyond all of that, we as a country are not producing nurses fast enough to keep up with the increasing health care needs of our aging population.”
The nurse shortage affects organizations across the spectrum of health care, not just St. Charles, which leads to the second part of the problem: St. Charles hospitals discharge many patients who need additional care to facilities known as SNFs, which stands for skilled nursing facilities – long-term acute care hospitals, inpatient rehab clinics, memory care facilities and other specialized services. But SNFs and other such post-acute facilities across Central Oregon are short-staffed and also at capacity, which means there is nowhere to send hospital patients who are being actively treated for acute injury and illness, including those who present to a St. Charles Emergency Department and are medically stabilized but require additional treatment as a hospital inpatient.
Meanwhile, St. Charles’ Emergency Department in Bend is busier than ever due to the usual increase in injuries and alcohol- and drug-related visits that come with summertime recreation and visitors to the region, as well as population growth. The Bend ED’s average daily census in past summers has been around 126 patients per day, said Michelle Brenholdt, the health system’s director of emergency services for Bend and Redmond. This summer, that number has jumped to 145 patients per day. Without appropriately staffed beds available in the hospital, some patients must stay in the ED – known as “boarding” patients – sometimes for days or weeks, using space, staff and other ED resources that are otherwise dedicated to people who present to the Emergency Department with medical emergencies.
“Every hospital in Oregon is boarding patients in the ED. Every hospital is backed up with patients awaiting transfers to post-acute care beds,” said Daniel Davis, senior director of patient flow for St. Charles. “We’re getting transfer requests from the coast and other places that are much farther away than usual. The situation is reflective of the challenges across the state.”
All of these bottlenecks – in the EDs, on hospital floors and in the SNFs – are exacerbated by the current surge of the Omicron BA.5 variant of COVID-19, which is highly contagious and prevalent in Central Oregon. The U.S. Centers for Disease Control has classified Deschutes, Crook and Jefferson counties as “high” transmission areas and is recommending that people wear masks when in crowded indoors settings to prevent the spread of the virus.
Following that recommendation would help slow the spread of COVID-19 and, in turn, help ease the pressure on Oregon hospitals. But it will not solve all the issues.
“Across the state and the country, health care is experiencing a crisis with regard to taking care of the communities we serve,” Merrill said. “This is a complicated mess we’re in, and there is no easy way out.”