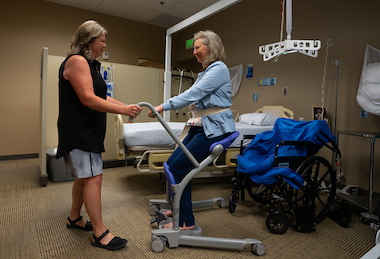
In the hospital, most of a patient's time is spent in bed. And during that time, muscle function can quickly ebb away. That's why movement and mobility are vital to recovery, whether a patient is resting during an extended treatment or recovering from surgery.
But mobility must be maintained in a way that is safe for patients and their providers. That's why St. Charles launched its Mobility is Medicine initiative last year.
"Mobility is part of medicine that you receive in the hospital," said Kelly Plunkett, a nurse manager in St. Charles' Intermediate Care Unit. "That's just as important as the pills and the treatment that you're getting here."
Inspired by a Johns Hopkins Medicine conference about mobility in hospitals, Plunkett and the health system’s injury prevention coordinator, Theresa Kramer, started infusing St. Charles with best practices for safe mobility in the spring of 2022. These practices center around preventing falls, decreasing pressure injuries in patients, and teaching providers how to aid patients' mobility without injuring themselves. (For example, if a nurse lifts a patient without the proper equipment, they can hurt their back.)
Made possible by several generous grants from the St. Charles Foundation, Plunkett and Kramer have secured numerous equipment upgrades that make movement safer and easier, such as bed slings.
“A lot of people think of a hospital stay as bedrest,” Kramer said, “but if you come to stay at St. Charles, you will be asked to move in a way that is safe for you.”
Across the organization, more than 600 nurses have been trained in safe mobility practices so far. In addition to training, the program also introduced a new bedside mobility assessment tool nurses can use to determine patients' mobility needs and the best ways to meet them.
Movement is a vital part of preventing secondary debilities that arise from patients spending more than 97% of their hospital time in bed, Kramer said.
"One of the themes we have been training is, 'Has my patient had their mobility medicine at least three times today?'" she said. "We’re trying to consciously put it in everybody's brain that there is an actual prescription for mobility so they get that it's just as important as a medication."
In the best-case scenario, mobility as medicine might be a patient getting up to walk three times in a day. But that isn't always possible, particularly if a person has suffered an extreme injury or trauma to the spine. In that case, providers may need to manually move patients' limbs to maintain muscles and promote blood flow.
While the training phase of the initiative recently wrapped up, it was just the beginning of the work, Plunkett said. In the coming months, the team will have enough preliminary data to track how effectively the program reduces patient and caregiver harm. Anecdotally, it seems to be making a dent in nurse injuries – a promising trend, given that health care workers are five times more likely to get hurt on the job than other professions.
"If we can get somebody assessed at the beginning and get them mobilized to their full potential every single day, that'll help get them out of the hospital sooner," Kramer said. "It's just so important."